If you’ve ever sought help for a mental or behavioral problem, it’s more than likely that you’ve received some form of Cognitive-Behavioral Therapy (CBT).
CBT is undoubtedly the most popular psychological intervention, with most psychologists, psychiatrists, and mental health nurses around the world practicing CBT or some variant of it.
This is for good reason, too, because CBT has been used to effectively treat numerous mental health conditions, ranging from depression, to anxiety, to eating disorders, to conduct disorders, and to substance abuse problems 1Tolin, D. F. (2010). Is cognitive–behavioral therapy more effective than other therapies?: A meta-analytic review. Clinical Psychology Review, 30, 710-720.
It should come as no surprise, then, that if you’re wanting to become a mental health professional, then one of the requirements in graduate school is demonstrating competency in CBT principles and techniques.
In this article, I want to provide a comprehensive overview of CBT.
Let’s get stuck into it.
Table of Contents
A Brief History of Cognitive-Behavioral Therapy
CBTs history stems from the early 1900’s, a time when psychoanalysis was the dominant approach to treating psychological problems.
The popularity of psychoanalysis quickly changed when behavioral theorists realized that psychological problems could be effectively addressed through pure behavioral exercises (rather than treating problems through unconscious forces) that stem from classical and operant condition principles, including systematic desensitization, imaginal exposure, and reinforcement contingencies.
Behavior therapy rapidly become successful around the 1940-50s for two primary reasons.
First, unlike psychoanalysis, behavior therapy had always taken an empirical approach, meaning that it allowed people to gather solid evidence on whether behavior therapy was or was not effective for alleviating mental health problems.
Second, behavior therapy was a far more economical treatment than psychotherapy.
In fact, less than 20 sessions of CBT can be more effective than 2 years of psychoanalysis 2Poulsen, S., Lunn, S., Daniel, S. I. F., Folke, S., Mathiesen, B. B., Katznelson, H., & Fairburn, C. G. (2014). A randomized controlled trial of psychoanalytic psychotherapy or cognitive-behavioral therapy for bulimia nervosa. The American Journal of Psychiatry, 171(1), 109-116. doi:10.1176/appi.ajp.2013.12121511!
That’s how long (or short) it can take for CBT to fully work.
Some people weren’t entirely happy with a pure behavioral approach, however. This was because behavior therapy paid no attention to a persons mental processes, such as their beliefs, interpretations, and cognitions.
They argued that a major reason why many people weren’t recovering from their mental health problems through behavior therapy was because no attention had been given to addressing any dysfunctional thought processes.
As a consequence, during the 1970’s a “cognitive revolution” emerged, wherein major psychologists’ tried to bring in cognitive phenomena into psychology and therapy.
Aaron Beck was at the forefront of this revolution; he began developing ideas about how to apply cognitive therapy in the 1960’s, which was then published into a book.
The first book on cognitive therapy, published in 1979, was written specifically for depression.
Over time, there was growing recognition that thoughts and behaviors go hand in hand – in other words, thoughts and behaviors both influence each other to a large extent.
This recognition forced people to combine pure behavior therapy with pure cognitive therapy to form the well-known cognitive-behavior therapy.
I think we can give Aaron Beck a lot of the credit for developing CBT.
Defining Cognitive-Behavior Therapy and its Principles
How can we define CBT?
It’s complicated – there’s no one single definition of CBT, and it’s surprisingly difficult to define. However, we can think of CBT as a collection of different therapeutic strategies that are each designed to correct faulty cognitive, behavioral, and emotional processes 3Hayes, S. C., Villatte, M., Levin, M., & Hildebrandt, M. (2011). Open, aware, and active: Contextual approaches as an emerging trend in the behavioral and cognitive therapies. Annual Review of Clinical Psychology, 7, 141-168. doi:10.1146/annurev-clinpsy-032210-104449.
This will make more sense when I touch on the principles that underlie CBT.
Here, I will set out the basic principles and beliefs of the CBT approach.
The Cognitive Principle
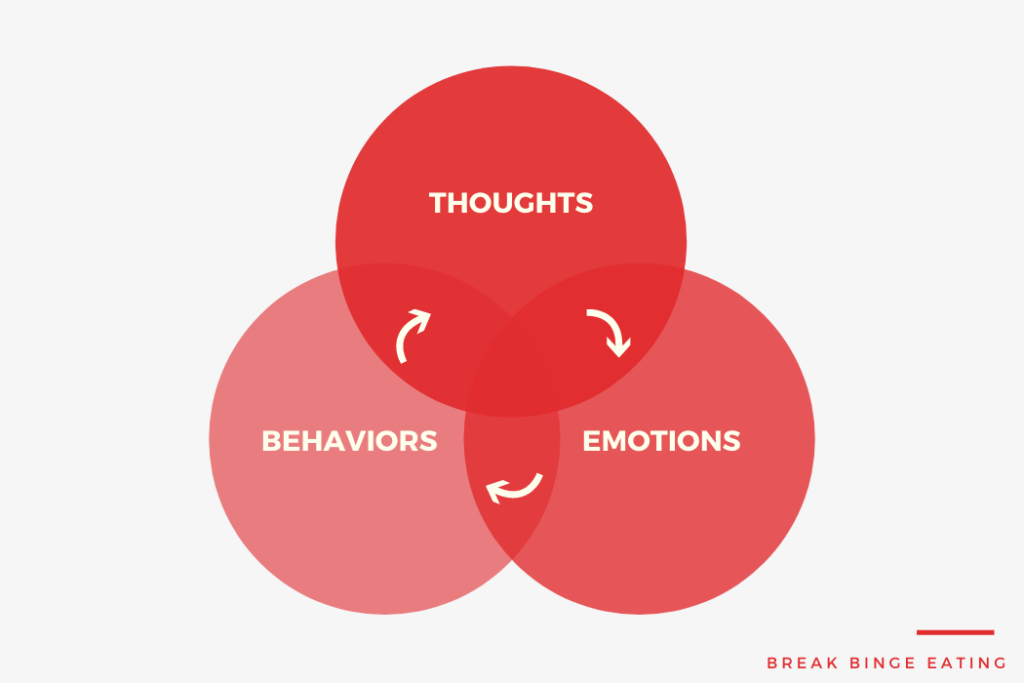
The cognitive principle means that CBT assumes that people’s emotions and behaviors are strongly influenced by cognitions 4Hofmann, S. G., & Asmundson, G. J. (2008). Acceptance and mindfulness-based therapy: new wave or old hat? Clinical Psychology Review, 28, 1-16. doi:10.1016/j.cpr.2007.09.003.
In other words, it is our interpretation, thoughts, and beliefs about something that will ultimate dictate how we will feel and how we behave towards ourselves, others, and the world.
Consider this: If we ask why someone is feeling angry, they will give us accounts of events or situations. For example, someone may say they are angry because they are stuck in traffic.
But, it can’t be that simple; if a situation like this automatically caused an emotion like anger in such a linear manner, then it would follow that the same event would have to result in the same emotion for everyone who experienced that event.
In other words, not everyone who sits in traffic gets angry, right?
No, people react differently to the same or similar event.
So, it’s not just the event that’s causing the emotion, but it’s also peoples interpretation, beliefs, or thoughts about the event that’s also influencing our emotions.
Paying attention to cognitions, particularly faulty or biased cognitions, is thus a central principle of CBT.
Let’s take a look at some of the more faulty cognitive processes people find themselves engaging – these cognitive processes are a large focus in CBT.
All-or-none thinking
People restrict possibilities and options of what they can think of only two choices.
Example: “I ate a piece of chocolate, so I completely failed my diet”
Overgeneralization
People view an isolated event as a continuing, never-ending pattern of defeat.
Example: “someone cut in front of me at the café, everyone always tries to push me around”
Negative mental filter
People dwell mostly on the negatives and ignore the positives.
Example: “Damn, I thought I would have lost more weight. I mean, I even beat my personal best time trial this week”
Discounting the positives
People are adamant that their achievements or positive efforts do not count.
Example: “Sure, I got the top grade in class, but it was only because the teacher made the test so easy for everyone”
Fortune-telling
People predict that things will turn out badly without any objective evidence.
Example: “I know that if I ask her out, she’ll laugh at me and reject me”.
Magnification
People blow things out of proportion or minimize their importance.
Example: “My best friend didn’t wave back at me before, he must hate me!”
Personalization
People blame themselves for something for which they weren’t entirely responsible.
Example: “If I only tried a little bit harder on the field, I guarantee my team would have won the game”.
In all of the above examples, we can see how these dysfunctional thinking styles can have an impact on our emotions and our behavior.
For example, consider the young boy who believes that he’ll get rejected if he asks a girl out on a date. His beliefs about this (that he will get rejected) will make him feel dejected, sad, or lonely, which in turn will cause him to avoid asking his crush on a date.
For these reasons, CBT will attempt to challenge the validity and content of this cognition in this boy. Changing this cognition is therefore expected to have a positive impact on his behavior and emotions.
This is how CBT works.
The Behavioral Principle
As the name states, CBT also pays close attention to peoples behaviors as well.
In fact, CBT considers behavior (what we do) as very important in maintaining or changing certain psychological states.
If we go back to example above, CBT would not only try to challenge the validity of this boy’s thoughts (the thought that he would get rejected), but it would also encourage the boy to test this thought by actively approaching the girl and asking her out.
He may find that the girl agrees to go on a date or that she expresses her gratitude but politely declines.
Either way, the behavior of approaching the girl will undoubtedly influence the boy’s emotions (e.g., pride or accomplishment for overcoming his fear) and thoughts (e.g., a sense of self-efficacy and confidence), which in turn will have a positive impact on his subsequent psychological functioning.
Ultimately, CBT believes that behavior can have a strong impact on thoughts and emotion, and, in particular, that changing what you do is often a powerful way of changing thoughts and emotions 5Hofmann, S. G., & Asmundson, G. J. (Eds.). (2017). The science of cognitive behavioral therapy. Academic Press.
The Continuum Principle
Contemporary medical approaches view mental health problems as pathological states that are qualitatively different from normal processes.
This view stands in contrast to CBTs continuum principle, which simply views mental health problems as arising from exaggerated or extreme versions of normal processes 6Westbrook, D., Kennerley, H., & Kirk, J. (2011). An introduction to cognitive behaviour therapy: Skills and applications. Sage Publications.
In other words, mental health problems, in CBTs view, are at one end of the continuum whereas normal mental processes are the opposite end – they are not on different dimensions altogether.
The Here and Now Principle
CBT is very different from many other psychological treatments in that its focus is on the present moment.
It largely ignores (not to say it doesn’t cover it at all) developmental processes, hidden motivations, and unconscious processes that are thought, by other theories, to contribute to psychological functioning.
Instead, its primary concern is on what keeping the psychological problem going, or what’s maintaining it.
The assumption follows that if we can address the primary factors that are responsible for “driving” the problem, then we should be able to eliminate the problem altogether.
For example, from CBTs perspective, depression is a consequence of certain faulty beliefs, interpretations, or thoughts people hold 7Beck, A. T. (Ed.). (1979). Cognitive therapy of depression. Guilford press.
A person may be chronically depressed because they believe that they’ve got nothing left to offer the world.
It is this belief that is maintaining the depression, and it is this belief that must be changed, according to CBT.
In this way, the main focus of CBT is on what is happening in the present moment, because this is believed to be the only true way to stop the core symptoms.
The Empirical Principle
A strong belief of the CBT approach is that we should be able to test theories and treatments through rigorous scientific method, rather than purely on clinical anecdote.
This principle explains why CBT advocates criticize psychoanalysts, as the psychoanalytic approach relies on unconscious processes that cannot be observed or measured. In other words, how and why would we change something if we are not entirely sure it exists in the first place?
Using the scientific method is important for a couple of reasons.
First, from an ethical standpoint, we can have confidence in telling people who are receiving our treatments that they are likely to be effective.
Second, from an economical stand-point, we can make sure that limited mental health resources are used in a way that will bring most benefit.
The Evidence of Cognitive-Behavior Therapy
CBT is the most widely studied psychological treatment in the world.
In fact, hundreds and hundreds of randomized controlled trials have been conducted evaluating the effectiveness of CBT for numerous mental health and behavioral problems across all age groups and multiple ethnic groups. These health problems range from:
- Depressive disorders
- Anxiety disorders
- Eating disorders
- Insomnia
- Substance use disorder
- Psychotic disorders
- Personality disorders
- Anger and aggression
- Chronic pain and fatigue
- Somatoform disorders
Dozens of systematic reviews and meta-analyses of CBT treatment studies have been published in recent years. In fact, there are even systematic reviews of systematic reviews on this topics 8Hofmann, S. G., Asnaani, A., Vonk, I. J., Sawyer, A. T., & Fang, A. (2012). The efficacy of cognitive behavioral therapy: A review of meta-analyses. Cognitive therapy and research, 36(5), 427-440.
Whilst it would take too much time going into detail of the findings from these, I’d like to highlight the key themes identified.
- CBT is substantially more effective than control conditions (that is, wait-lists, pill-placebo, care as usual) for most problems listed above
- CBT is more effective than other specific psychological treatments, like interpersonal therapy, mindfulness therapy, and psychodynamic therapy, for certain conditions like eating disorders, anxiety disorders, and depressive disorders.
- CBT is most effective when the treatment is delivered individually by a therapist, rather than in self-help or group format.
- CBT is equally effective to pharmacological treatments for depression, anxiety, and eating disorders.
Frequently Asked Questions About Cognitive-Behavior Therapy
Let’s address a couple of common questions people might ask about CBT.
How long does Cognitive-Behavior Therapy (CBT) take?
Therapists usually deliver CBT according to a treatment manual. Although there are no clear “rules” for how long CBT should go for, the treatment typically lasts somewhere between 16-24, 50 minutes sessions with a therapist.
However, there is actually little evidence to suggest that “more is better”. In other words, more sessions do not equate to better outcomes!
In fact, 8 sessions of CBT may be equally effective to 20 sessions of therapy.
This is why CBT gives us bang for our buck!
How much does Cognitive-Behavior Therapy (CBT) cost?
There isn’t a straightforward answer; obviously it depends on the type of therapist you see, how long you see them for, and the demand for that therapist.
In Australia, for example, one session of CBT can cost anywhere between $80 to $250.
Do I have to see a therapist for Cognitive-Behavior Therapy (CBT)?
Not necessarily.
The beauty of CBT is that it can be translated for delivery through technology (the Internet, smartphone apps) or self-help books.
This means that you can receive CBT at almost no cost!
And what’s most impressive is that dozens of studies have shown that CBT delivered through the computer, phone, or books can be highly effective for those mental health problems mentioned above 9Andrews, G., Basu, A., Cuijpers, P., Craske, M., McEvoy, P., English, C., & Newby, J. (2018). Computer therapy for the anxiety and depression disorders is effective, acceptable and practical health care: an updated meta-analysis. Journal of anxiety disorders.
But, outcomes seem to be best when people receive some level of support from a professional 10Linardon, J., Cuijpers, P., Carlbring, P., Messer, M., & Fuller-Tyszkiewicz, M. (2019). The efficacy of app-supported smartphone interventions for mental health problems: a meta-analysis of randomized controlled trials. World Psychiatry, 18, 325-336. doi:10.1002/wps.20673.
11 Best Cognitive-Behavior Therapy (CBT) Books
Let’s break this down a bit.
First, I’ll provide the references to some good books that talk about CBT, its origin, principles, evidence, and techniques for a range of mental health problems.
- Persons, J. B. (2012). The case formulation approach to cognitive-behavior therapy. Guilford Press.
- Craske, M. G. (2014). Cognitive-behavioral therapy. American Psychological Association.
- Fairburn, C. G. (2008). Cognitive behavior therapy and eating disorders. Guilford Press.
- Beck, A. T. (Ed.). (1979). Cognitive therapy of depression. Guilford press.
- Butler, G., Fennell, M., & Hackmann, A. (2010). Cognitive-behavioral therapy for anxiety disorders: Mastering clinical challenges. Guilford Press.
- Westbrook, D., Kennerley, H., & Kirk, J. (2011). An introduction to cognitive behaviour therapy: Skills and applications. Sage.
- Hofmann, S. G., & Asmundson, G. J. (Eds.). (2017). The science of cognitive behavioral therapy. Academic Press.
Now, I’ll provide some useful self-help books that are based on CBT. These books contain step-by-step strategies on how to overcome that particular problem, often accompanied by CBT worksheets.
- Fairburn, C. G. (2013). Overcoming binge eating: The proven program to learn why you binge and how you can stop. Guilford Press.
- Gilbert, P (2009). Overcoming depression: A self-help guide using cognitive behavioral techniques: Hachette UK.
- Williams, C (2012). Overcoming anxiety, stress, and panic. A five areas approach. CRC press.
- Shafran R, Ega, S & Wade, T (2018). Overcoming perfectionism: A self-help guide using scientifically supported cognitive behavioral techniques. Robinson
References

Great article !!! You said “it is our interpretation, thoughts, and beliefs about something that will ultimate dictate how we will feel and how we behave towards ourselves, others, and the world”
So, how can I change a limiting thought or belief ? Do you have a step by step system about it ???